Unveiling the core science of Chronic Constipation and Gastroparesis, exposing medication pitfalls and the exercise paradox to restore gut balance and vitality.
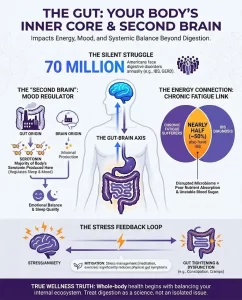
Reacquainting Yourself with Your Digestive System
Have you ever been troubled by slow digestion, post-meal bloating, or difficulty having a bowel movement? These seemingly minor discomforts not only impact your daily comfort but may also quietly erode your internal well-being. To fix this, we’ve often followed “common sense” advice: eat more vegetables, drink more water, and exercise more.
However, a core concept is often overlooked: much of the widely circulated “common sense” may not apply to everyone, and can even be counterproductive. For example, blindly increasing fiber intake sometimes fails to relieve constipation and instead worsens bloating and discomfort. This stems from a widespread misunderstanding of how the digestive system truly operates.
This article will delve into the often-ignored fundamental causes behind slow digestion—from neurological command and medication influence to the subtle balance of exercise intensity—to reveal a science-based, gentle, and effective set of solutions. Our goal is to help you move beyond reliance on short-term “laxative fixes” toward achieving long-term inner gut balance.
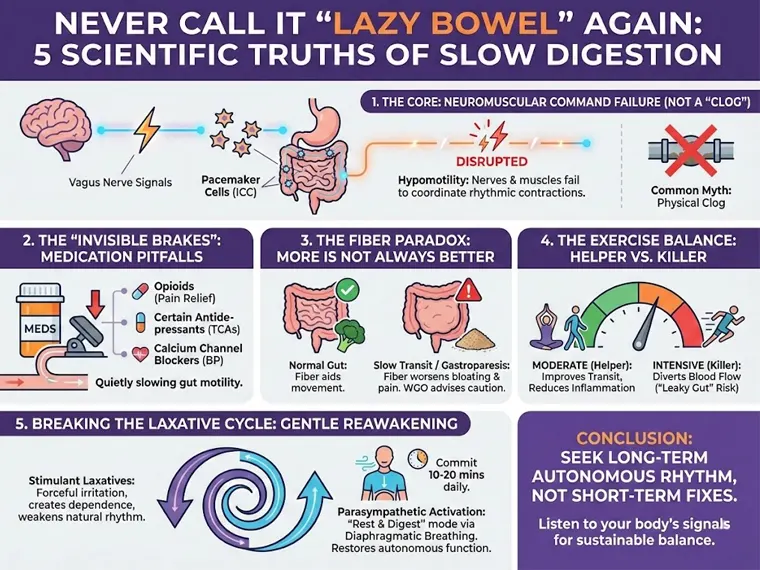
5 Disruptive Insights into Slow Digestion
1. The Key is “Motility,” Not Just “Movement“: Rethinking the Nerve and Muscle Command System
We often picture slow digestion and constipation as a physical “clog,” but the essence is often a neuromuscular dysfunction, specifically gastrointestinal hypomotility. The movement of food through the digestive tract relies on a sophisticated nerve and muscle command system, not simple gravity or pressure.
According to the Mayo Clinic and related scientific literature, the rhythmic contractive movements (peristalsis) of the gastrointestinal (GI) tract depend on signals from the vagus nerve and coordination by Interstitial Cells of Cajal (ICC), often referred to as the digestive tract’s “pacemaker cells.” This system acts as the “commander” and “metronome” of digestion, ensuring food is ground, digested, and transported at the correct speed.
However, various factors can damage this command system. For instance, long-term diabetes, viral infections, or even unexplained autoimmune reactions can impair the vagus nerve, leading to delayed gastric emptying (Gastroparesis) or Slow Transit Constipation (STC).
The World Gastroenterology Organisation (WGO) further categorizes chronic constipation into different types—normal transit, slow transit, and defecatory disorders—underscoring the problem’s complexity. Understanding this is crucial: the focus of the solution must shift from mere “clearing the block” to supporting nervous system health and restoring muscle function. This is the root-cause approach.
2. Review Your Medicine Cabinet: The “Invisible Brakes” That Quietly Slow Your Gut
Another often-overlooked cause is that many common medications used to treat other conditions may be the very culprits slowing your digestive system. They act as the gut’s “invisible brakes” without you realizing it.
Based on data from the World Gastroenterology Organisation and academic research, the following common drug classes are significantly associated with an increased risk of constipation:
- Opioid Pain Relievers: Such as Morphine and Codeine.
- Certain Antidepressants: Especially tricyclic antidepressants (TCAs) like Amitriptyline.
- Calcium Channel Blockers: Often used for high blood pressure, such as Verapamil.
- Iron and Calcium Supplements: Common nutritional supplements.
- Diuretics: Used to treat edema or high blood pressure.
Given that Adverse Drug Reactions (ADR) are a significant concern, with approximately 10% being GI-related, if you suffer from chronic digestive issues and are taking multiple prescription or over-the-counter medications, it is highly recommended to carefully review your list with a doctor or pharmacist for potential links. Sometimes, adjusting the medication regimen can bring unexpected improvement in gut motility.
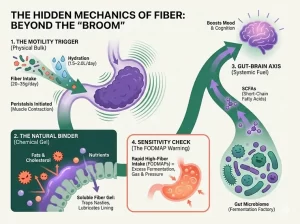
3. The Fiber Paradox: Why “Eating More Veggies” Might Worsen Your Trouble
“Eat more fiber for constipation” is almost universal health advice. However, this advice holds a significant paradox: for certain types of slow digestion, increasing fiber intake can actually aggravate the problem.
WGO guidelines explicitly state that fiber supplements should be avoided in patients with defecatory disorders or obstructive bowel diseases. Similarly, an article from Medical News Today explains that for patients with Slow Transit Constipation (STC), whose bowels lack sufficient motility to propel stool, increasing fiber only adds bulk that the body cannot expel, thereby worsening bloating, abdominal pain, and discomfort.
Furthermore, for individuals with Gastroparesis, Mayo Clinic experts often recommend a low-fiber diet because fiber can further delay already sluggish gastric emptying, causing food to remain in the stomach longer.
This is not to negate the value of fiber, but to stress its suitability. The correct approach is to introduce fiber gradually and ensure sufficient water intake. If your bloating, abdominal pain, or gas symptoms worsen after increasing fiber, it may be a crucial signal that your issue is not simply a lack of fiber, but a more complex motility disorder that requires medical consultation.
4. The Exercise Balance Rule: How Intensity Decides If It’s a “Helper” or a “Killer”
The impact of exercise on gut health is significantly bidirectional. Moderate exercise is a “helper” that promotes bowel movement, while excessive, strenuous exercise can become a “killer.”
A systematic review clearly indicates that regular moderate-intensity exercise—such as brisk walking, yoga, or cycling—can effectively improve gut transit time, reduce systemic inflammation, and is highly beneficial for relieving constipation and symptoms of Irritable Bowel Syndrome (IBS).
However, the review also warns that high-intensity or long-duration exercise (like marathon running) can cause a phenomenon called splanchnic hypoperfusion. In this state, the body redirects a large volume of blood away from the digestive tract to prioritize working muscles. This lack of blood flow (ischemia) can lead to damage to the intestinal lining, increase gut permeability (“leaky gut“), and trigger or worsen acute GI symptoms like abdominal pain, nausea, and diarrhea.
The key is finding the exercise “sweet spot” tailored to your personal physical condition. Learn to listen to your body’s signals, especially when feeling digestive discomfort. Avoid high-intensity training and opt for gentle activities like walking to promote circulation while maintaining the stability of the digestive system.
5. Breaking the “Laxative Dependence“: Gently Reawakening the Gut’s Own Rhythm
When bowel movements are difficult, many people resort to laxatives. However, chronic dependence, especially on stimulant laxatives (like senna or bisacodyl), creates a vicious cycle: the more they are used, the more dependent the gut becomes, and its own function grows increasingly “lazy.”
Stimulant laxatives work by forcing the bowels to contract through nerve and muscle irritation. Over time, the bowel develops tolerance and dependence on this external stimulus, weakening its ability to contract autonomously.
In contrast, a more scientific and sustainable approach is to awaken the gut’s inherent healthy rhythm. Relaxation techniques recommended by the International Foundation for Gastrointestinal Disorders (IFFGD) offer a gentle yet effective path. Through practices like diaphragmatic breathing, we can consciously influence the autonomic nervous system and activate the parasympathetic nervous system—the one responsible for “rest and digest.” When the parasympathetic system is activated, heart rate slows, muscles relax, and the motility and secretion functions of the digestive tract are naturally enhanced.
You can try the following simple relaxation exercise guide, committing 10-20 minutes daily:
- Preparation: Sit comfortably in a supportive chair or lie down in a quiet, peaceful environment. Ensure your head is well-supported and your body is still and symmetrical.
- Facial Relaxation: Gently close your eyelids, feeling the muscles around your eyes completely relax. Your lips and teeth should be slightly parted, allowing your jaw to drop naturally.
- Body Relaxation: Let your shoulders drop naturally and relax. Feel your hands resting gently on the armrests or your thighs, fingers naturally curled. Keep your feet still, toes facing outward, forming a natural “V” shape.
- Diaphragmatic Breathing: Focus your attention on your breath. Adopt a slow, deep, and rhythmic breathing pattern. As you inhale, feel your abdomen gently expand like a balloon; as you exhale, feel it naturally contract.
- Maintain the State: Stay in this quiet, relaxed state. If your thoughts wander, simply and gently bring your attention back to the rhythm of your breath.
The goal of such practice is not to intervene forcefully but to regulate the nervous system, creating an ideal working environment for the gut, helping it restore its autonomous, healthy internal rhythm.
The Modern Life Efficiency Gap and Scientific Solutions
Through the above analysis, it is clear that digestive system health is far more complex than just a “quick fix.” It is a precise system engineering project involving nerve command, drug influences, dietary wisdom, exercise balance, and stress management.
However, in fast-paced modern life, perfectly executing all these gentle lifestyle adjustments—precisely calculating fiber intake, maintaining the right exercise intensity, adhering to daily relaxation training, and ensuring nutritional balance—is a significant challenge for many. This is the “Modern Efficiency Gap“: we know the right direction but lack the time and energy for continuous execution.
It is precisely to bridge this gap that science-based auxiliary tools have emerged. They are not intended to replace a healthy lifestyle or act as potent stimulant laxatives, but rather as scientific, efficient aids to better support the body’s natural functions within limited time constraints.
The So Easy 3-Day Cleanse Program: A Gentle and Highly Effective Support Plan
The core philosophy of the So Easy 3-Day Cleanse Program is to provide a gentle yet highly efficient support solution for the body. It does not rely on stimulating ingredients to force bowel movements but is a nutritionally balanced meal replacement plan that supports the gut’s natural detoxification and repair process by allowing it to “rest and recuperate” for three days.
The most unique scientific component of the plan is its oil palm fiber. Unlike traditional fibers (like psyllium husk) that promote defecation by increasing stool bulk, oil palm fiber’s mechanism is one of “lubrication” rather than “scraping” or “forceful stimulation.” It can penetrate and soften the viscous mucoid plaque that has adhered to the intestinal wall for a long time, making it easier to naturally detach and slide out. This gentle method avoids the bloating, abdominal pain, and discomfort often caused by traditional high-fiber products, with many users reporting the process as “effortlessly sliding out.”
As its philosophy states: “Why wait thirty days when it can be done in three?” This reflects its efficiency in the context of modern life while ensuring a gentle and comfortable experience.
Furthermore, the program includes three functional phases—Detoxification, Repair, and Nourishment. This means it is more than just cleaning; it is a complete support system. During the cleanse, it provides essential amino acids, vitamins, minerals, and energy, ensuring the body does not lack necessary nutritional support while it is “resting.”
Conclusion: Seeking Long-Term Balance Over Short-Term Quick Fixes
The true key to resolving slow digestion issues lies in deeply understanding their complex root causes and adopting multi-faceted, sustainable, and gentle strategies. Whether it’s adjusting diet structure, optimizing exercise habits, managing stress, or, when necessary, utilizing a science-based auxiliary plan like So Easy, the ultimate goal should be unified: to help the body restore its natural, healthy, and autonomous functional rhythm.
Remember, our body is a precise system full of wisdom. Instead of using forceful means to fight symptoms, learn to be a keen observer of your own body, listening to and understanding every signal it sends. The road to long-term inner balance begins with awareness, is nurtured by gentleness, and is perfected through consistency.
What challenges have you faced or what effective methods have you discovered in managing your digestive health? Share your story in the comments section below.