Unlocking the profound connection between gut health and skin clarity. Why topical care fails, and how root-cause action provides a lasting, radiant glow.
Introduction
Are you frustrated by the constant recurrence of acne, inflammation, and redness, despite investing in countless expensive skincare products? If topical solutions aren’t solving the core issue, the answer might be deep inside your body.
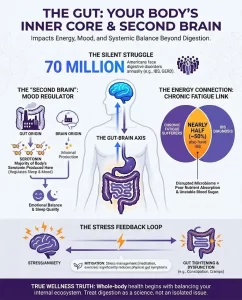
Scientific research increasingly highlights the critical link known as the gut-skin axis—a bidirectional communication highway connecting gastrointestinal health and skin stability. Rather than merely being the mirror of your gut, your skin is the final, most visible chapter of the internal story. When gut health is compromised, the skin is often the first place to show signs of distress.
An imbalance in the gut microbiota (known as dysbiosis) can damage the gut barrier, triggering a low-grade, persistent systemic inflammation. This inflammation ultimately “erupts” through the skin. This is precisely why focusing on gut health is crucial for managing skin problems. This article will reveal five science-backed truths that may completely change your perspective, giving you the knowledge and power to achieve clear skin from the source.
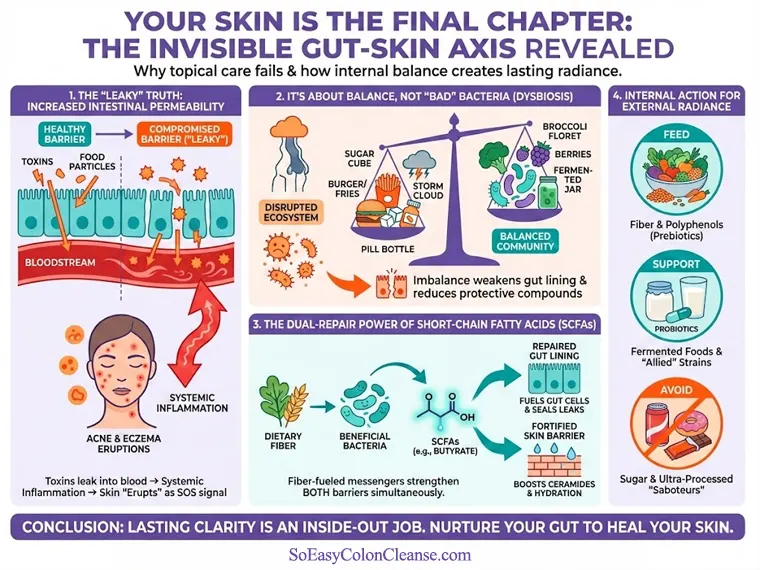
1. Beyond “Leaky Gut”: A Scientific Look at Increased Intestinal Permeability
You’ve likely heard the term “leaky gut syndrome” circulating in wellness circles. However, it’s important to clarify that “leaky gut” itself is not a recognized medical diagnosis. The popular term describes a very real scientific phenomenon: increased intestinal permeability.
The inner lining of the gut is supposed to be a selective barrier, permitting only water and essential nutrients to pass through. When this barrier is compromised, its permeability increases, allowing large molecules that should not enter the bloodstream—such as toxins, partially digested food particles, and bacterial metabolites—to “leak” into circulation.
This condition is often a result of chronic inflammation, which can be triggered by underlying diseases like Inflammatory Bowel Disease (IBD) or Celiac Disease, or by factors like a poor diet, chronic stress, or the overuse of Non-Steroidal Anti-Inflammatory Drugs (NSAIDs).
2. Your “Bad” Bacteria Aren’t the Enemy—Gut Dysbiosis is the Key
Many people believe that “bad” bacteria in the gut are the enemy and must be completely eradicated. The truth is, a healthy gut depends on a diverse and balanced microbial community, not the absence of certain bacteria. The core issue is not a battle between “good” and “bad,” but the state of the entire ecosystem’s balance.
When this balance is disrupted, it leads to gut dysbiosis. This is commonly caused by several factors:
- Poor Diet: Diets high in refined sugar, saturated fat, and ultra-processed foods selectively promote the growth of microbes that thrive on simple sugars and fats, essentially “starving” the beneficial bacteria that rely on fermentable dietary fiber to produce helpful compounds.
- Stress: Chronic psychological stress can directly impact the composition and function of the gut microbes via the brain-gut-skin axis.
- Antibiotics: While killing pathogenic bacteria, antibiotics can non-discriminately wipe out large numbers of beneficial bacteria, destabilizing the gut’s ecosystem.
Gut dysbiosis leads to two major problems: first, it exacerbates damage to the gut barrier, leading to the increased intestinal permeability mentioned earlier; second, it reduces the generation of beneficial metabolites. This imbalance not only directly damages the gut lining but also weakens the production of key compounds that actively defend and repair this barrier—a crucial mechanism we’ll explore next.
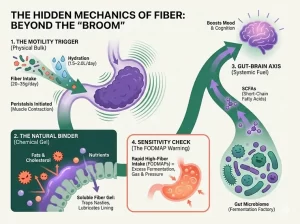
3. The Unsung Heroes: How Short-Chain Fatty Acids (SCFAs) Repair Your Dual Barriers
In the connection between gut health and clear skin, one class of molecules acts as vital messengers: Short-Chain Fatty Acids (SCFAs). These key metabolic byproducts, most notably butyrate, are generated when beneficial gut bacteria ferment the dietary fiber we consume.
SCFAs, especially butyrate, possess powerful dual-repair functions, simultaneously strengthening both the gut and the skin barriers:
- For the Gut: Butyrate is the preferred energy source for colon cells. It fuels the cells lining the gut, helping to maintain the integrity of the intestinal barrier, reduce permeability, and prevent “leaking.”
- For the Skin: SCFAs that enter the bloodstream from the gut have been shown to fortify the skin’s physical barrier by promoting the differentiation of keratinocytes and boosting the production of essential structural components, such as ceramides and filaggrin.
By strengthening these two barriers, SCFAs fundamentally reduce the systemic inflammation that triggers skin issues.
4. The Inflammation Link: Skin Issues Are Concentrated “SOS Signals” from the Gut
Now, let’s connect the dots to clearly illustrate how gut issues escalate into conditions like acne, atopic dermatitis (eczema), and psoriasis on the skin. The process is a chain reaction:
- Gut Dysbiosis: Poor diet, stress, and other factors lead to a decrease in beneficial bacteria and an increase in harmful ones.
- Compromised Gut Barrier: Increased intestinal permeability allows bacterial toxins and inflammatory molecules to enter the bloodstream.
- Systemic Inflammation: These foreign substances activate the body’s immune system, generating low-grade, chronic inflammation throughout the body.
- Skin Manifestation: This systemic inflammation eventually shows up through the skin—the body’s “window“—leading to acne, redness, eczema flares, and dryness.
Specific research backs this connection. For instance, studies on atopic dermatitis patients found a significant reduction in the amount of a beneficial bacterium called Faecalibacterium prausnitzii. This is crucial because F. prausnitzii is one of the most important species for producing the anti-inflammatory substance butyrate. Its decrease directly correlates with other findings: the gut environment of atopic dermatitis sufferers is severely compromised in its ability to generate this key barrier-fortifying compound.
5. Skin Wellness from Within: 3 Actionable Steps for Gut Health
Understanding the science is one thing; taking action is another. Here are three simple, effective, and science-based action plans to help you improve your skin by nurturing your gut.
Action 1: Feed Your Beneficial Microbiome
- Consume Enough Dietary Fiber: Your beneficial bacteria require “food” to produce Short-Chain Fatty Acids. Ensure your diet is rich in soluble and insoluble fiber from vegetables, fruits, legumes, and whole grains.
- Eat Polyphenol-Rich Foods: Blueberries, green tea, and dark chocolate are high in polyphenols, which are powerful antioxidants that also promote microbial diversity in the gut.
Action 2: Supplement with “Allied” Probiotics
- Eat Fermented Foods: Fermented foods like yogurt with live cultures, kefir, and sauerkraut are natural sources of probiotics, helping to re-balance the gut microbiota.
- Consider Specific Probiotic Strains: Research suggests that specific strains of the Lactobacillus and Bifidobacterium genera are excellent for reducing inflammation and supporting skin health.
Action 3: Avoid “Internal Saboteurs”
- Reduce intake of added sugars, artificial sweeteners, and ultra-processed foods. These ingredients feed harmful bacteria, exacerbate gut dysbiosis, and fuel inflammation.
A Deep Reset for Your Gut
Long-term dietary adjustment is fundamental, but sometimes our digestive system needs a powerful reset to clear accumulated waste and lay the foundation for rebuilding a healthy gut environment. If you feel sluggish, have dull skin, and crave a complete internal cleanse, a targeted, efficient program can help you start a new chapter.
The So Easy 3-Day Cleanse Program is designed as a targeted solution for this purpose. Its unique advantage is that it is one of the only cleanse products on the market utilizing oil palm fiber. This specific fiber effectively lubricates the colon wall, gently yet powerfully aiding in the removal of hardened, long-standing fecal matter—referred to by the product as mucoid plaque (a term used to describe the buildup of hardened mucus and fecal material).
By helping to clear this accumulated waste, the program aims to lower the body’s overall inflammatory load. As per the core message of this article, the reduction in systemic inflammation is the mechanism behind users’ reported experience of clearer, more radiant skin (a “glow“), directly improving acne and blemishes, and resulting in a smoother, cleaner skin texture. This is more than just a cleanse; it’s a three-day, nutritionally balanced meal replacement plan that allows your digestive system to rest and repair while your body receives essential nutrients.
Conclusion
Achieving lasting skin clarity is an inside-out job, intricately tied to the long-term balance of your gut. While topical products have their place, they cannot resolve inflammation that originates internally. Focusing on gut health through diet and lifestyle may not be an instant fix, but it is the sustainable path toward truly healthy skin.
Now that you understand the gut’s language, what is your skin telling you it needs from within?
Share your favorite gut-friendly foods or skincare tips in the comments below!