Unlocking 4 Counterintuitive Gut Health Truths and Practical Strategies for Long-Term Digestive Balance.
Introduction: Rethinking the Age-Old Advice to “Eat More Greens”
If you’ve ever struggled with irregularity, bloating, or constipation, you are certainly not alone. You’ve likely tried all the common recommendations: increasing your vegetable and fruit intake. But why do these methods sometimes offer minimal relief, or even make things worse? The answer lies in a widespread knowledge gap. Achieving sustained healthy bowel movements is about far more than just adding fiber. You will learn that, under specific conditions, a high-fiber diet lacking sufficient water can turn from a solution into the very source of your discomfort. This article will reveal four science-based insights that challenge conventional wisdom, helping you avoid common pitfalls and build truly effective habits for long-term gut comfort and balance.
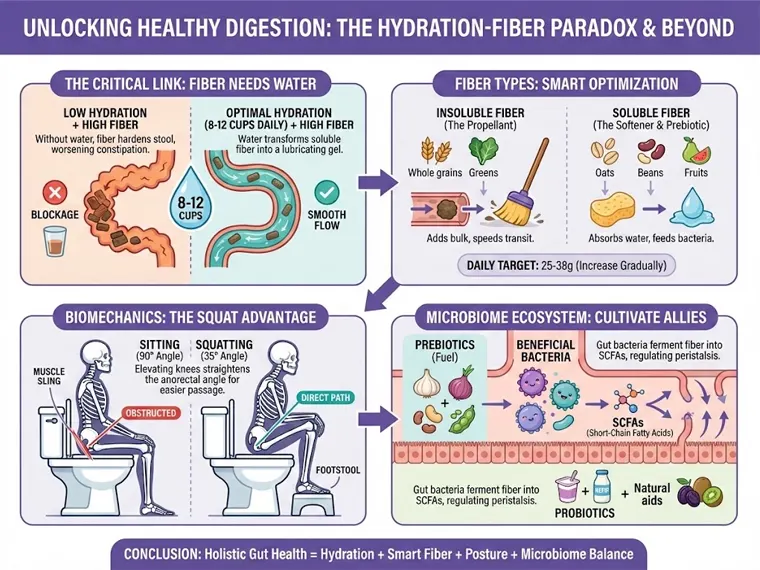
Strategy One: Optimizing Dietary Fiber – Focus on Type, Not Just Quantity
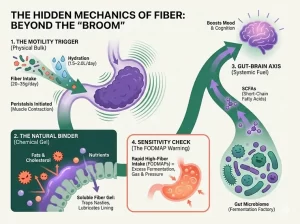
Simply increasing your dietary fiber intake without considering its type and your body’s adaptability is often the main culprit behind bloating and gas. Understanding the differences in how various fibers work is the first step toward digestive health.
Insoluble Fiber: The Gut’s “Propellant“
Insoluble fiber acts as a physical “bulking agent.” It does not dissolve in water and remains mostly intact in the digestive tract, mechanically stimulating the intestinal wall to speed up peristalsis by increasing the physical volume of the stool—like a “propellant.” Major sources include whole grains (like wheat bran) and non-starchy vegetables.
Soluble Fiber: The Gut’s “Softener” and “Prebiotic“
Soluble fiber is fundamentally different. It dissolves in water to form a gel-like substance, effectively binding and holding moisture. This makes it act as a “softener,” ensuring stools are softer and easier to pass. Crucially, soluble fiber is the primary “food” for your gut microbiome. Scientific research indicates that stool is largely composed of bacteria. Therefore, feeding your beneficial bacteria with soluble fiber effectively increases the stool’s biomass while keeping it soft and well-hydrated. Excellent sources include oats, beans, legumes, nuts, and most fruits.
Scientific Fiber Intake Strategy
To consume fiber “smartly,” follow these science-backed strategies:
- Define Your Goal: Scientific consensus suggests a daily fiber target of 25-30 grams for adult women and 30-38 grams for adult men.
- Increase Gradually: Rapidly increasing fiber intake can stress the digestive system. Be sure to increase it incrementally, allowing your digestive tract and gut microbiome ample time to adapt, thereby preventing abdominal discomfort.
- Prioritize High-Density Sources: For efficient daily goal achievement, prioritize foods with high fiber density:
| Food Source | Serving Size | Total Fiber Content (Grams) |
| Split Peas (cooked) | 1 cup (approx. 7 oz.) | 16.0 |
| Lentils (cooked) | 1 cup (approx. 7 oz.) | 15.5 |
| Black Beans (cooked) | 1 cup (approx. 6 oz.) | 15.0 |
| Chia Seeds | 1 ounce (approx. 28 grams) | 10.0 |
Dietary fiber exhibits a homeostatic regulatory effect: when stool is too hard, it binds water to soften it, relieving constipation; when stool is too loose, it increases volume and form.
Strategy Two: Optimizing Hydration – The True Key to Bowel Motility
This is the most critical and counterintuitive point of the article: in the absence of adequate hydration, a high-fiber diet is not only ineffective but can worsen constipation. Dehydration is a well-established cause of hard, dry stool that is difficult to pass. Soluble fiber works by absorbing water to form a gel; if your body lacks water, the fiber will draw moisture from the already limited water in your colon, resulting in stool that is even drier, harder, and more difficult to move.
Scientific Benchmark for Daily Water Intake
According to the official recommendations from the U.S. National Academies of Sciences, Engineering, and Medicine, the average daily total fluid intake (including water from food) is about 15.5 cups (3.7 liters) for men and 11.5 cups (2.7 liters) for women. For a more actionable target aimed at relieving constipation: aim to drink 8-12 cups of water daily. This ensures that dietary fiber can perform its optimal lubricating and softening roles.
What You Drink Also Matters
Note that not all liquids are beneficial. Limit the intake of alcohol and caffeinated beverages, as they can have a diuretic effect, causing your body to lose more water through urine and working against your hydration goals.
Strategy Three: Optimizing Defecation Posture – A Neglected Biomechanical Trick
The design of modern toilets, while comfortable, conflicts with our body’s natural defecation mechanism. At the end of our rectum, a muscle called the puborectalis muscle loops around it like a sling. When we adopt a standard sitting posture, this muscle is only partially relaxed, creating a curved “kink” that obstructs the smooth passage of stool.
The Science of Squatting
The solution is simple: elevate your knees above your hips using a small footstool, simulating a natural squatting posture. This small change allows the puborectalis muscle to fully relax, straightening the anorectal angle and creating a direct, unobstructed channel for stool. Scientific studies have clearly demonstrated that adopting this posture significantly reduces the time required for a bowel movement and decreases the need for abdominal pressure and straining.
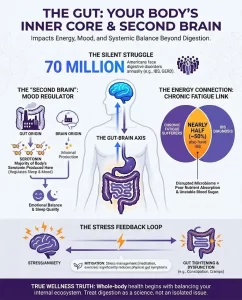
Strategy Four: Optimizing the Gut Microbiome – Cultivating Your “Bowel Allies”
The foundation of gut health lies in maintaining a balanced microbial ecosystem. Our gut bacteria are not passive; they actively participate in and finely regulate peristalsis by fermenting dietary fiber to produce Short-Chain Fatty Acids (SCFAs). This regulatory effect is complex: SCFAs can both stimulate intestinal cells to release serotonin, promoting bowel motility, and stimulate other cells to release hormones like GLP-1 and PYY, inhibiting it. This exquisite dual-regulation mechanism ensures balanced and coordinated bowel movement.
Providing “Fuel” for Probiotics: The Power of Prebiotics
Prebiotics are food components that are selectively fermented by beneficial bacteria in our gut (particularly Bifidobacteria and Lactobacilli). They are the exclusive fuel for these “allies,” promoting their growth and proliferation. Natural food sources rich in prebiotics include:
- Garlic
- Onions
- Asparagus
- Legumes
- Barley
Directly Supplementing “Allies“: Sources of Probiotics
Probiotics are the live, beneficial microorganisms themselves. By consuming probiotic-rich fermented foods, we can directly supplement the gut with these powerful “allies.” Excellent sources include:
- Yogurt (containing active cultures)
- Kefir
- Sauerkraut
- Kimchi
Clinical evidence demonstrates that prebiotics are effective in alleviating constipation, primarily by increasing the number of beneficial bacteria, particularly Bifidobacteria and Lactobacilli. [Source: National Institutes of Health]
Clinically Validated Natural Functional Foods
Beyond macro-strategies, certain specific natural foods show strong laxative effects due to their unique composition.
- Prunes: Prunes are a first-line natural treatment for constipation. Their effectiveness stems from the synergistic action of three mechanisms: high levels of soluble and insoluble fiber, sorbitol (which draws water into the colon via osmosis), and polyphenols (which nourish the gut microbiome). Randomized clinical trials have even shown that consuming 50-100 grams (about 6-12 prunes) daily is more effective at increasing spontaneous bowel movements than the common fiber supplement, psyllium husk.
- Kiwifruit: Kiwifruit is an excellent choice for those prone to bloating from high fiber or sorbitol. Studies prove that consuming two green kiwifruit daily has comparable constipation relief effects to prunes or psyllium husk, but its key advantage is a significant reduction in adverse reactions like bloating, leading to higher patient satisfaction.
When You Need a Strong Start: A Unique Natural Support
While establishing the long-term habits discussed above, our bodily system sometimes needs a gentle “reset” or a structured push to clear accumulated waste and get back on track. For those who feel their colon is chronically “backed up,” considering structured support options is a reasonable choice.
Unique Assistance from Oil Palm Fiber
In this context, some products, such as the So Easy 3-Day Colon Cleanse program, offer unique support. According to their product literature, core ingredients include oil palm fiber and guar gum. Interestingly, guar gum is a type of soluble fiber consistent with the scientific consensus: it forms a gel with water in the gut, softening stool and adding bulk. Furthermore, the product highlights its unique oil palm fiber, claiming its primary mechanism is to lubricate the colon walls, creating a smooth channel that helps accumulated fecal matter slide out easily.
The Differentiating Factor
The product’s marketing materials contrast it with common fiber supplements. While conventional fiber supplements like psyllium are clinically used as effective bulk-forming laxatives, primarily adding volume by absorbing water, the So Easy program proposes a different mode of action. According to its creators, oil palm fiber aims to penetrate and “un-stick” long-adhered matter. The program is designed to provide a gentle experience, avoiding the bloating or cramping that other products might cause. As per official documentation, the program aims to clear what they term mucoid plaque and cleanse the entire digestive system, setting a foundation for a healthy gut environment.
Conclusion: The Holistic Path to Long-Term Gut Balance
Achieving persistent gut health and smooth, healthy bowel movements is not dependent on a single “magic pill” or method. It is a comprehensive, long-term balance strategy that requires patience and wisdom. The four core strategies revealed in this article—smart fiber optimization, ensuring optimal hydration, adopting the correct defecation posture, and cultivating a healthy gut microbiome—collectively form the scientific blueprint for achieving this goal. Consistent adherence to these physiologically and biomechanically sound habits will bring long-term benefits far exceeding your expectations.
Having learned these science-backed strategies, which one will you try first today to better listen to your body?
Share Your Thoughts
Share your experiences in the comments, or tell us what other secrets you know for maintaining gut health! We look forward to your insights.